
How to Reduce Your Risk of Sports Injuries: Essential Prevention Strategies
Whether you’re an amateur enthusiast or a seasoned athlete, sports injuries can be a major setback. However, with the right prevention strategies, you can significantly

Chiropractic care with both direction and magnitude

Whether you’re an amateur enthusiast or a seasoned athlete, sports injuries can be a major setback. However, with the right prevention strategies, you can significantly

Whether you’re an aspiring amateur or a seasoned professional, enhancing athletic performance is a common goal among all athletes. You might have tried various training

If you’re a weekend warrior, you likely spend your weekdays anticipating the physical activities that the weekend promises. Whether it’s playing basketball, going for long
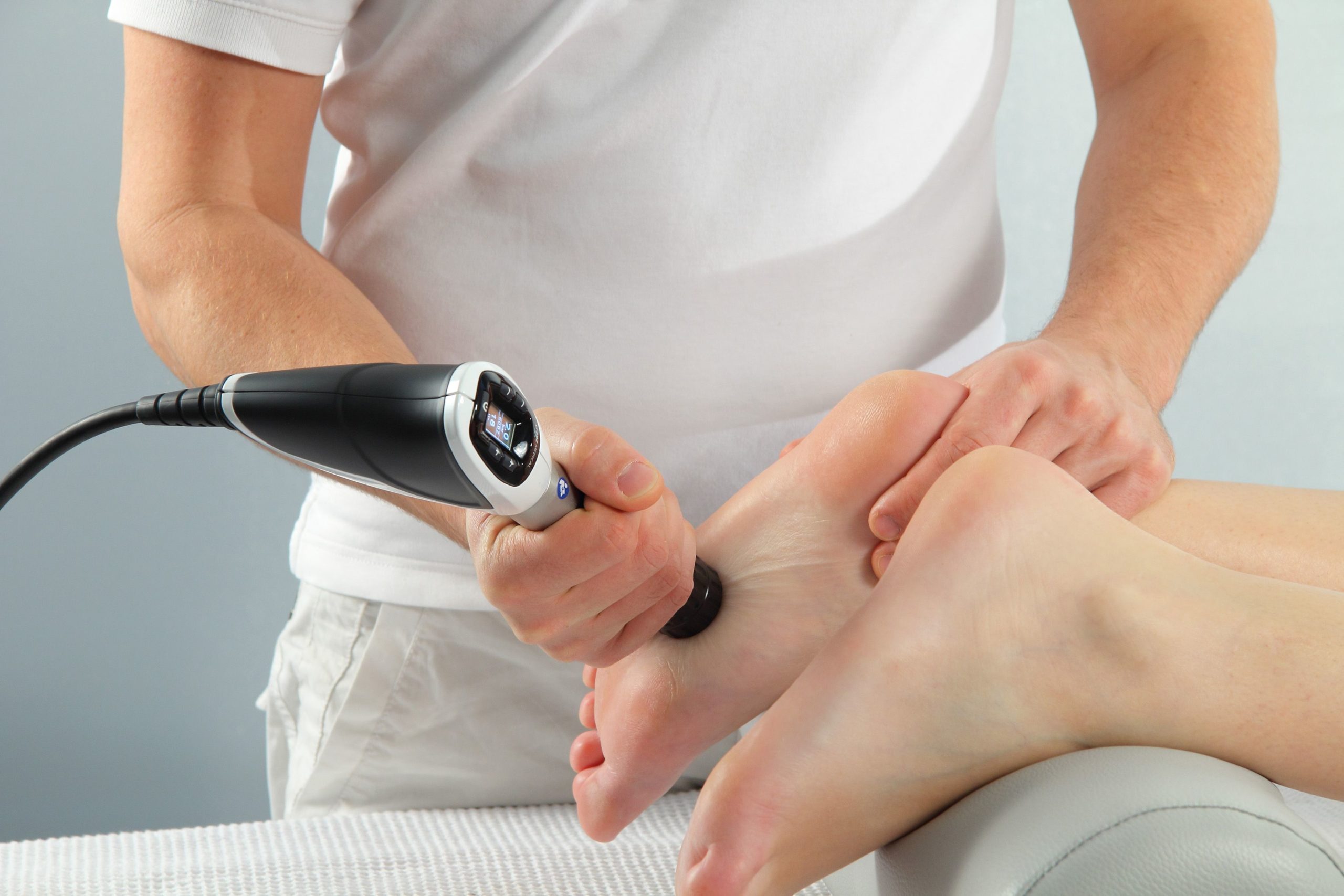
Introduction Rehabilitation plays a vital role in helping individuals recover from injuries, manage chronic conditions, and regain their quality of life. Over the years, various
The following information is from a great book meant for the non-physician to help resolve their own back problems. The book is by Stuart McGill

Knee pain is a common complaint in many populations. The common conditions can cause knee pain. learn more and talk you your local Millcreek UT Chiropractor

Elbow pain can have many causes. Golfers elbow, tennis elbow are the common names for lateral and medial epicondylitis. Which is caused by irritation of

When it comes to the shoulder the most common injuries or conditions are sprains and strains, rotator cuff tears, tendonitis, bursitis, arthritis. The shoulder is

What is an Ankle Sprain? An ankle sprain is injuries that occur when the ankle rolls, twists, and or turns, and the body is not

What is Plantar Fasciitis? It is one of the most common causes of heel pain according to the Mayo clinic. It involves inflammation of the